10 Tips to Prevent Bedsores
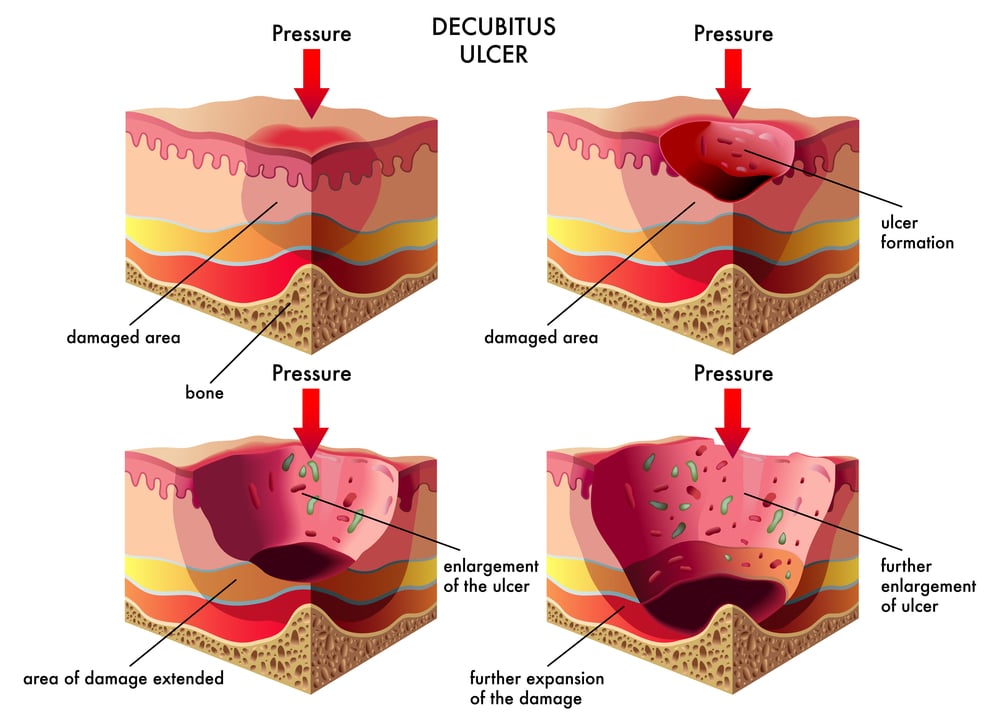
Bedsores — also called pressure ulcers and decubitus ulcers — are injuries to skin and underlying tissue resulting from prolonged pressure on the skin. Bedsores most often develop on skin that covers bony areas of the body, such as the heels, ankles, hips, and tailbone.
People most at risk of bedsores are those with a medical condition that limits their ability to change positions or those who spend most of their time in a bed or chair.
Bedsores can develop quickly. Most sores heal with treatment, but some never heal completely. You can take steps to help prevent bedsores and aid healing.
Table of Contents
Here are 10 tips to prevent bedsores
Tip # 1
Several risk assessment tools like the Braden scale help determine the patient’s risk of developing pressure ulcerations (bedsores). One of the best ways to prevent and treat pressure ulcers is to document the risk assessment clearly.
Tip # 2
Examine the patient’s skin regularly and look for any signs of damage. Non-blanching erythema is often the first sign of tissue damage. In addition to this, look for other signs such as swelling, heat, or induration.
Tip # 3
Ensure the skin is kept clean, hydrated, and dry to help decrease the risk of damage to the skin. Carefully pat dry the skin and avoid rubbing the skin, as friction can damage skin.
Tip # 4
Excess moisture can damage the skin. Incontinent patients are at an increased risk of developing bedsores. Take appropriate measures to keep the patient’s skin dry. Use barrier creams and incontinence pads to help keep the patient dry. Finally, catheters should only be considered a last resort because of the risk of infection.
Tip # 5
Excess perspiration in the folds of the skin can also increase the risk of bedsores. Choose lightweight, breathable clothing to help minimize excess perspiration.
Tip # 6
Nutrition is essential to prevent and heal skin ulcers. Assess the patient’s diet and address any nutritional needs promptly. Furthermore, ensure the patient is properly hydrated to help improve the skin’s elasticity and condition.
Tip # 7
The patient’s position should also be considered when trying to prevent ulcers. If the patient is unable to change their position themselves, medical personnel should change the patient’s position regularly to reduce the risk of bedsores.
Tip # 8
Ergonomics are essential to a patient’s comfort and can help them perform everyday tasks. Consider the placement and size of each piece of furniture, including the patient’s chairs, mattress, and bed.
Tip # 9
The patient must be able to reposition themselves often. If the patient cannot complete this themselves, make sure medical personnel respect their patient’s privacy, comfort, and dignity when repositioning a patient.
Tip # 10
There is pressure redistributing equipment that can help reduce the risk of bedsores. This equipment helps to increase comfort while redistributing pressure. Pressure-reducing cushions and a pressure relieving mattress should always be used in patients at a high risk of developing bedsores.